Depressants
Last published: June 06, 2025
What are depressants?
Depressant substances reduce arousal and stimulation. They affect the central nervous system, slowing down the messages between the brain and body.1
They can affect concentration and coordination and slow down a person’s ability to respond to unexpected situations. In small doses, they can cause a person to feel more relaxed and less inhibited.1
In larger doses they can cause drowsiness, vomiting, unconsciousness and death.2
How are depressant drugs used?
How they’re used depends on the specific type of depressant. For example, alcohol is drunk and benzodiazepines are usually swallowed - but they can also be injected.
Generally, depressants can be swallowed, drunk, injected, snorted or inhaled.
Commonly used depressants
Explore depressants on the Drug Wheel
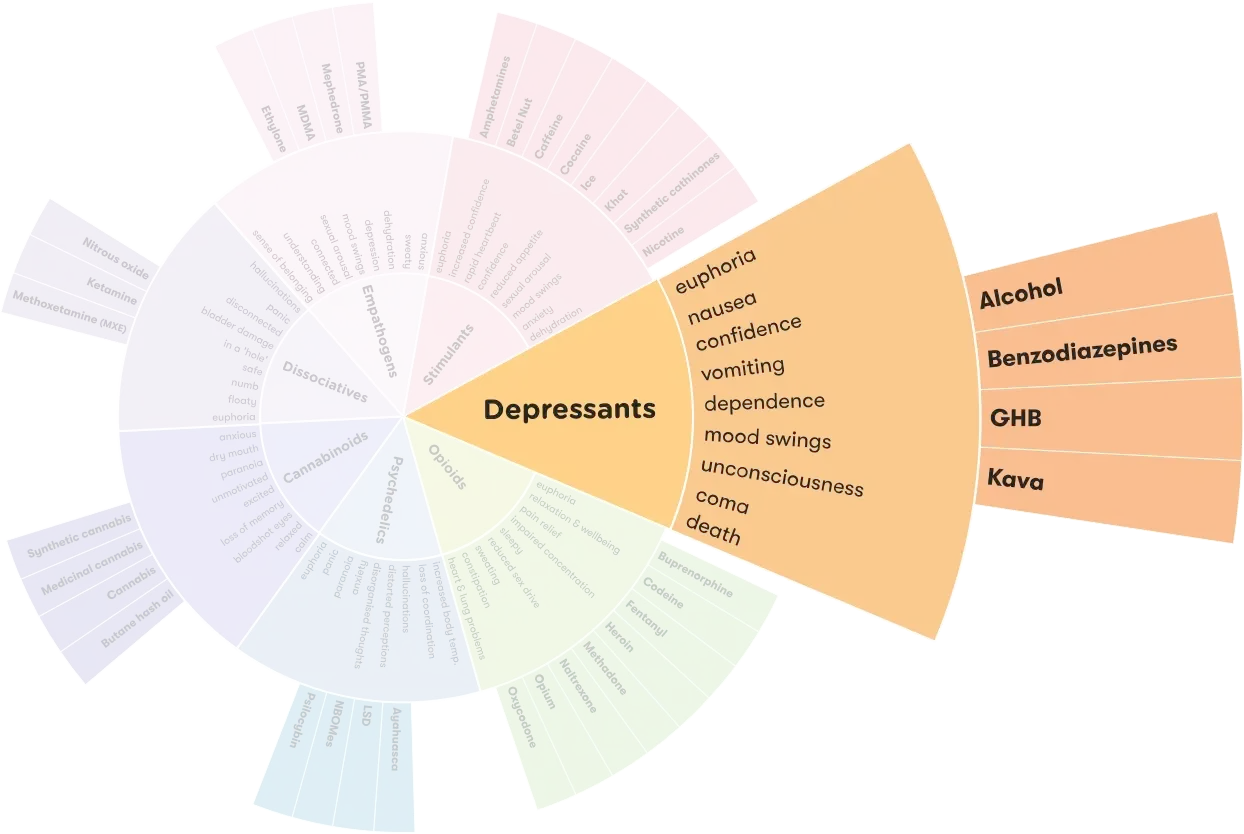
Effects of depressants
Use of any drug can have risks. It’s important to be careful when taking any type of drug.
Depressants affect everyone differently, based on:
- size, weight and health
- whether the person is used to taking it
- whether other drugs are taken around the same time
- the amount taken
- the strength of the drug (this varies from batch to batch with illegally produced drugs).
The onset and effects of depressants vary according to the type and specific chemical.
Some depressants may work instantly, with effects only lasting for a short time (such as inhalants). While for other depressants, it may take longer for the effects to start and may be slower to wear off.
In general, when small to low doses of depressants are taken, the following effects may be experienced:
- reduced inhibitions
- enhanced mood
- reduced anxiety and stress
- slowed reaction time
- impaired judgement
- slowed breathing
- increased risk of accident or injury.1
Higher doses can result in:
- impaired judgement and coordination
- vomiting
- irregular or shallow breathing
- blackouts and memory loss
- unconsciousness
- coma
- death.1
Overdose
If you take a large amount or have a strong batch, you could overdose.
Call an ambulance straight away by dialling triple zero (000) if you have any of the following symptoms:
- vomiting
- awake but not responsive
- limp body
- pale or clammy face
- blue fingernails or lips
- slow breathing or not breathing at all
- slow heartbeat
- choking or gurgling sounds
- unconsciousness.1
Mixing depressants with other drugs
The effects of taking depressants with other drugs – including over-the-counter or prescribed medications – can be unpredictable and dangerous.
- Alcohol + benzodiazepines: decreased heart rate and breathing; overdose more likely.3
- Benzodiazepines + opiates (such as heroin): breathing difficulties; an increased risk of overdose and death.3
Use of more than one drug or type of drug consumed at the same time is called polydrug use.4
More on Polydrug use
Polydrug use is a term for the use of more than one drug or type of drug at the same time or one after another. Polydrug use can involve both illicit drugs and legal substances, such as alcohol and medications.
Health and Safety
Use of depressants is likely to be more dangerous when:
- combined with alcohol or other drugs, particularly
- driving or operating heavy machinery
- judgement or motor coordination is required
- a person is alone (in case medical assistance is required).
Use of any drug always carries some risk, however, if you choose to take it, always try a small test amount first.4 For example, the chemical composition of GHB/GBL is highly variable. It’s very easy to take too much GHB - the difference between the amount needed to get high and the amount that causes an overdose can be hard to judge.
If drinking alcohol, stay hydrated and have something to eat before and while drinking.
Tolerance and dependence
People who use depressants regularly, can develop a dependence and tolerance to them. Tolerance means they need to take larger amounts of depressants to get the same effect.
People who are psychologically dependent may feel an urge to use them when in specific surroundings or socialising with friends. With physical dependence, a person’s body adapts to the depressants and gets used to functioning with them.
People who depend on depressants may find that using the drug becomes more important than other activities in their life. Cravings can make it difficult to stop using depressants.
Reducing harm
Use of depressants is likely to be more dangerous when:
- combined with alcohol or other drugs, particularly
- driving or operating heavy machinery
- judgement or motor coordination is required
- a person is alone (in case medical assistance is required).
Use of any drug always carries some risk. But, if you choose to take it, always try a small test amount first.4 For example, the chemical composition of GHB/GBL is highly variable. It’s very easy to take too much GHB - the difference between the amount needed to get ‘high’ and the amount that causes an overdose can be hard to judge.
If drinking alcohol, stay hydrated and have something to eat before and while drinking.
Withdrawal
Giving up depressants after using them for a long time is challenging because the body has to get used to functioning without them.
The severity of withdrawal symptoms will depend on the type of depressant, but generally withdrawal symptoms should settle down in about 5-7 days.
Withdrawal symptoms vary from person to person, but generally the withdrawal from depressants may include:
- cold or flu-like symptoms
- headache
- sweating
- aches and pains
- difficulty sleeping
- nausea
- mood swings7
Getting help
If your use of depressants is affecting your health, family, relationships, work, school, financial or other life situations, or you’re concerned about someone else, you can find help and support.
Call the National Alcohol and Other Drug Hotline on 1800 250 015 for free and confidential advice, information and counselling about alcohol and other drugs
Help and Support Services search
Find a service in your local area from our list. Simply add your location or postcode and filter by service type to quickly discover help near you.
If you're looking for other information or support options, send us an email at [email protected]
Path2Help
Not sure what you are looking for?
Try our intuitive Path2Help tool and be matched with support information
and services tailored to you.

- Brands B, Sproule B, Marshman J, Ontario. Addiction Research F. Drugs & drug abuse : a reference text. Toronto, Ont.: Addiction Research Foundation; 1998 [cited 2021 May].
- Australian Government Department of Health. Types of Drugs - Drug catagories 2019 [12.01.2021].
- Kang M, Galuska M, Ghassemzadeh S. Benzodiazepine Toxicity. Treasure Island (FL): StatPearls Publishing; 2020.
- Darke S, Lappin J, Farrell M. The Clinician's Guide to Illicit Drugs. United Kingdom: Silverback Publishing 2019.
- World Health Organization. Lexicon of alcohol and drug terms 2021 [19.03.2021].
- Black E. Polydrug use: What you need to know about mixing drugs. In: National Drug and Alcohol Research Centre UoNSW, editor. 2014.
- Gowing L, Ali R, Dunlop A, Farrell M, Lintzeris N. National Guidelines for Medication-Assisted Treatment of Opioid Dependence. Department of Health 2014 [25.08.2020].