Types of benzodiazepines
There are three types of benzodiazepines: long, intermediate and short-acting. Short-acting benzodiazepines have stronger withdrawal or ‘come down’ effects and can be more addictive than long-acting ones.2
Benzodiazepines are known by their chemical (generic) name or their brand name. In each case the drug is the same – it’s just made by a different company. Some common benzodiazepines are:
Pharmaceutical names
| Generic name | Brand name | Type |
|---|---|---|
| diazepam | Ducene®, Valium® | Long-acting |
| lorazepam | Ativan® | Short-acting |
| oxazepam | Alepam®, Murelax®, Serepax® | Short-acting |
| nitrazepam | Alodorm®, Mogadon® | Intermediate-acting |
| temazepam | Euhypnos®, Normison® | Short-acting |
| alprazolam | Xanax®, Kalma®, Alprax® | Short-acting |
Adapted from: Brands B, Sproule B & Marshman J. (eds) (1998) Drugs & Drug Abuse (3rd ed.) Ontario: Addiction Research Foundation.
How are they used?
Benzodiazepines are usually swallowed. Some people also inject them.
Effects of benzodiazepines
Use of any drug can have risks. It’s important to be careful when taking any type of drug.
Benzodiazepines affect everyone differently, but the effects may include:
- reduced stress
- euphoria
- reduced anxiety
- calmness
- depression
- confusion
- feelings of isolation or euphoria
- impaired thinking and memory loss
- headache
- drowsiness, sleepiness and fatigue
- dry mouth
- slurred speech or stuttering
- double or blurred vision
- impaired coordination, dizziness and tremors
- nausea and loss of appetite
- diarrhoea or constipation.1
Injecting benzodiazepines may also cause:
- vein damage and scarring
- infection, including hepatitis B, hepatitis C, HIV and AIDS
- deep vein thrombosis and clots which can result in loss of limbs, damage to organs, stroke and possibly death.5
Injecting drugs repeatedly and sharing injecting equipment with other people increases the risk of experiencing these effects.4
Who are benzodiazepines not recommended for?
Benzodiazepines are not recommended for use during pregnancy or breastfeeding, as they are associated with pre-term delivery, low birth weight and potential birth defects.5-7
They may also be dangerous for people with:
- acute asthma, emphysema or sleep apnoea
- advanced liver or kidney disease
- or people with a history of substance use disorders, as their use can lead to dependence.8,9
Benzodiazepines taken by elderly people can increase their risk of falls and injury.
Overdose
Benzodiazepines are often present in patients who have intentionally or accidentally overdosed.
If you take a large amount or mix them with other drugs, you could overdose.
Call triple zero (000) and request an ambulance if you or someone else has any of the following symptoms (emergency services are there to help and can provide instructions over the phone).
Symptoms include:
- over-sedation or sleep
- jitteriness and excitability
- mood swings and aggression
- slow, shallow breathing
- unconsciousness or coma
- death (more likely when taken with another drug such as alcohol).3
Long-term effects
Regular use of benzodiazepines may cause:3,11
- impaired thinking or memory loss
- anxiety and depression
- irritability, paranoia and aggression
- personality change
- weakness, lethargy and lack of motivation
- drowsiness, sleepiness and fatigue
- difficulty sleeping or disturbing dreams
- headaches
- nausea
- skin rashes and weight gain
- dependence
- withdrawal symptoms (see below).3
There is some evidence that long-term, heavy use of benzodiazepines is a risk factor for epilepsy, stroke and brain tumours.12
Using benzodiazepines with other drugs
The effects of taking benzodiazepines with other drugs − including over-the-counter or prescribed medications − can be unpredictable and dangerous.
Benzodiazepines + alcohol or opiates (such as heroin): breathing difficulties, an increased risk of overdose and death.6, 7
Benzodiazepines + some pharmaceutical drugs: strong pain-relievers, antidepressants, anticonvulsants, anti-psychotics, some anti-histamines and over-the-counter medications can have an adverse effect when taken with benzodiazepines and lead to breathing difficulties, an increased risk of overdose and death.7, 8
The use of benzodiazepines to help with the come down effects of stimulant drugs (such as amphetamines or ecstasy) could result in a cycle of dependence on both types of drug.
Use of more than one drug or type of drug consumed at the same time is called polydrug use.10
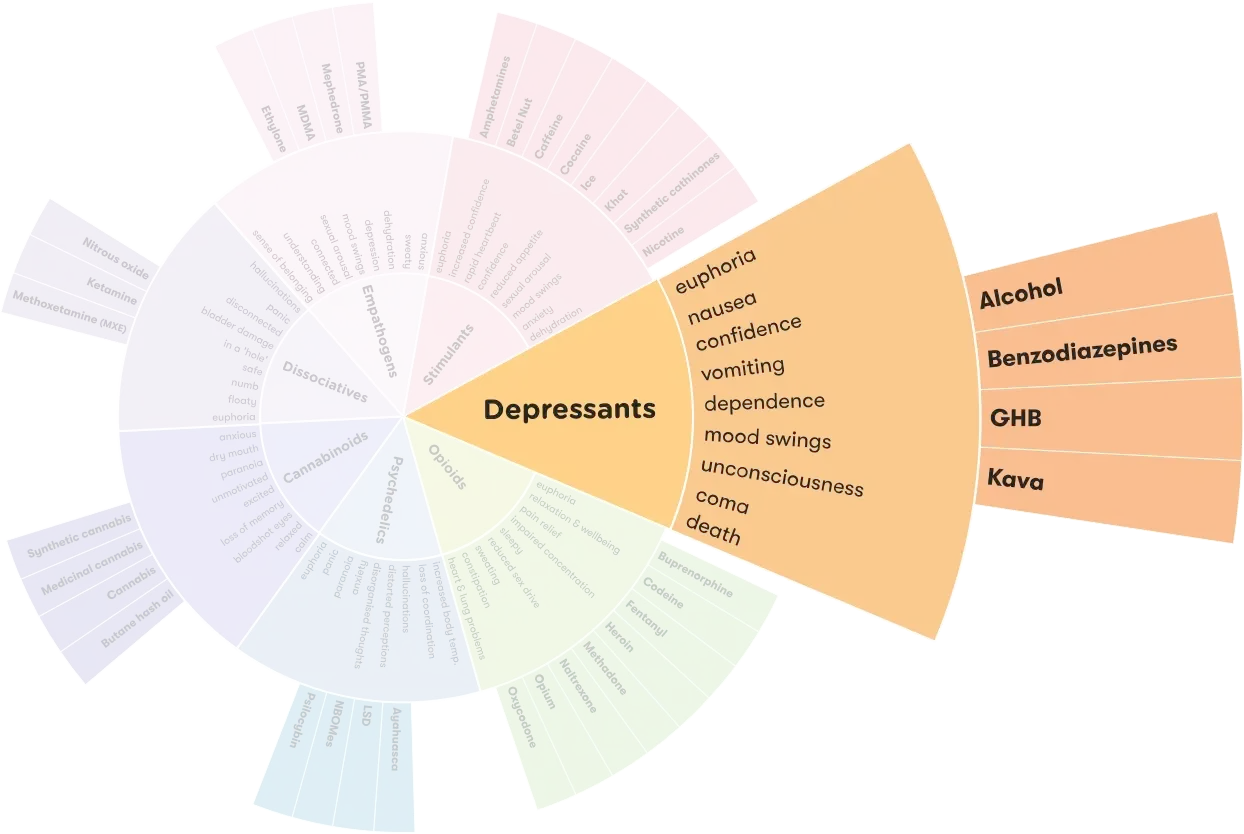
More on Polydrug use
Polydrug use is a term for the use of more than one drug or type of drug at the same time or one after another. Polydrug use can involve both illicit drugs and legal substances, such as alcohol and medications.
Reducing harm
- Use somewhere safe and around people you trust.
- Avoid mixing with other drugs especially alcohol and opioids.
- Do not use more than recommended or by your prescriber.
- Only use short term as dependence can develop rapidly.
- If injecting, use a clean needle and syringe each time.
- If snorting, crush to a fine powder as large chunks can cause cuts and bleeding.
- Avoid driving or operating machinery if taking benzos.
Novel benzodiazepine
Australia is seeing increased availability of novel benzos as people look for new drug experiences or street alternatives to controlled prescription medicines.9
There is limited information on the short and long-term health effects of novel benzodiazepines, but we know that:
- Novel benzos can have similar effects to prescribed benzos but can be stronger and more unpredictable.
- Novel benzos often have similar chemical structures to prescribed benzos.10
- Novel benzos may vary in strength from batch to batch, and even from tablet to tablet, which increases the risk of toxic effects because the dose cannot be accurately gauged.11
- Novel benzos may contain different drugs (including opioids) and other substances and fillers.12
- Between 2015-2021 there were 40 overdose deaths involving novel benzos in Australia.13
- And in Victoria, there’s been a sharp increase in deaths from novel benzos - from one in 2018; to 10 in 2019; and, 28 in 2020.11
- There have been a number of health alerts in Australia about fake Xanax, Kalma and Mylan.12
Withdrawal
Giving up benzodiazepines after a long time is challenging because the body has to get used to functioning without them. So it’s important to seek advice from a health professional when planning to stop taking benzodiazepines. If taking benzodiazepines is suddenly stopped, sudden withdrawal can cause seizures.4,10
Withdrawal symptoms vary from person to person and are different depending on the type of benzodiazepine being taken. Symptoms can last from a few weeks to a year and can include:
- headaches
- aching or twitching muscles
- dizziness and tremors
- nausea, vomiting, stomach pains
- bizarre dreams, difficulty sleeping, fatigue
- poor concentration
- anxiety and irritability
- altered perception, heightening of senses
- delusions, hallucinations and paranoia
- seizures.3
Getting help
If your use of benzodiazepines is affecting your health, family, relationships, work, school, financial or other life situations, or you’re concerned about someone else, you can find help and support.
Call the National Alcohol and Other Drug Hotline on 1800 250 015 for free and confidential advice, information and counselling about alcohol and other drugs
Help and Support Services search
Find a service in your local area from our list. Simply add your location or postcode and filter by service type to quickly discover help near you.
If you're looking for other information or support options, send us an email at [email protected]
Path2Help
Not sure what you are looking for?
Try our intuitive Path2Help tool and be matched with support information
and services tailored to you.

In Australia, using benzodiazepines without a prescription from a doctor, or selling or giving them to someone else, is illegal.
There are also laws against forging or altering a prescription or making false representation to get benzodiazepines or a prescription for them.11
In 2014, in response to concerns about the use and harms associated with the benzodiazepine alprazolam (Xanax®), it was rescheduled under the Pharmaceutical Benefits Scheme (PBS) as a Schedule 8 drug. Doctors must now follow additional state and territory laws when prescribing alprazolam and must notify, or receive approval from, the appropriate health authority.12
National
4.7% of Australians aged 14 years and over have used tranquillisers/sleeping pills (including benzodiazepines) for non-medical purposes one or more times in their life.13
1.6% of Australians aged 14 years and over have used tranquillisers (including benzodiazepines) for non-medical purposes in the previous 12 months.13
Young people
Young Australians (aged 14–24) first try tranquilisers for non-medical purposes at 18.2 years on average.14
- Brands B Sproule B Marshman J. Drugs & Drug Abuse. 3rd ed. Ontario: Addiction Research Foundation; 1998.
- Darke S, Lappin, J. & Farrell, M. The Clinician's Guide to Illicit Drugs. United Kingdom: Silverback Publishing 2019.
- Ritter A, King T, Hamilton M. Drug use in Australian society. South Melbourne, Vic.: Oxford University Press; 2017 [cited 2021 May]. Available from:
- The Royal Australian College of General Practitioners. Prescribing drugs of dependence in general practice, Part B – Benzodiazepines Melbourne, Australia: The Royal Australian College of General Practitioners; 2015 [04.03.2022].
- Preston A Derricott J. The Safer Injecting Handbook 2017.
- Liang D, Shi Y. Prescription drug monitoring programs and drug overdose deaths involving benzodiazepines and prescription opioids. Drug and alcohol review [Internet]. 2019 [cited 2021 June]; 38(5):[494-502 pp.].
- Knopf A. Why mixing alcohol, opioids and benzodiazepines can kill. Alcoholism & Drug Abuse Weekly [Internet]. 2020 [cited 2021 June]; 32(6):[5 p.].
- Upfal J. Australian drug guide : the plain language guide to drugs and medicines of all kinds. Melbourne, Vic.: Black Inc.; 2016 [cited 2021 June]. Available from:
- United Nations Office on Drugs and Crime. Understanding the synthetic drug market: the NPS factor. 2018.
- Moustafa R, Tarbah F, Saeed H, Sharif S. Designer benzodiazepines versus prescription benzodiazepines: can structural relation predict the next step? Critical Reviews in Toxicology. 2021;51(3).
- Coroners Court Victoria. Finding into Death without Inquest_COR 2021 002418. 2021.
- NSW Health. Fake Kalma alprazolam tablets found to contain strong opioids 2022 [cited: October 2022].
- Darke S, Peacock A, Duflou J, Farrell M, Lappin J. Characteristics of fatal 'novel' benzodiazepine toxicity in Australia. Forensic Sci Int. 2022.
- Fluyau D, Revadigar N, Manobianco BE. Challenges of the pharmacological management of benzodiazepine withdrawal, dependence, and discontinuation. Therapeutic Advances in Psychopharmacology [Internet]. 2018 2018/05/01 [cited 2021 June]; 8(5):[147-68 pp.]. Available from:
- DRUGS, POISONS AND CONTROLLED SUBSTANCES ACT 1981 - SECT 36B, (n.d.).
- Australian Government Department of Health. Prescribing Medicines – Information for PBS Prescribers 2022 03.05.2022].
- Australian Institute of Health and Welfare. National Drug Strategy Household Survey detailed report 2016. Canberra AIHW; 2017.
- Guerin N, White V. Australian secondary school students’ use of tobacco, alcohol and other drugs in 2017. Melbourne, Victoria: Cancer Council Victoria; 2020 [cited 2021 May].
Path2Help
Not sure what you are looking for?
Try our intuitive Path2Help tool and be matched with support information
and services tailored to you.