How are amphetamines used?
Amphetamines are generally snorted, swallowed, injected or smoked.6
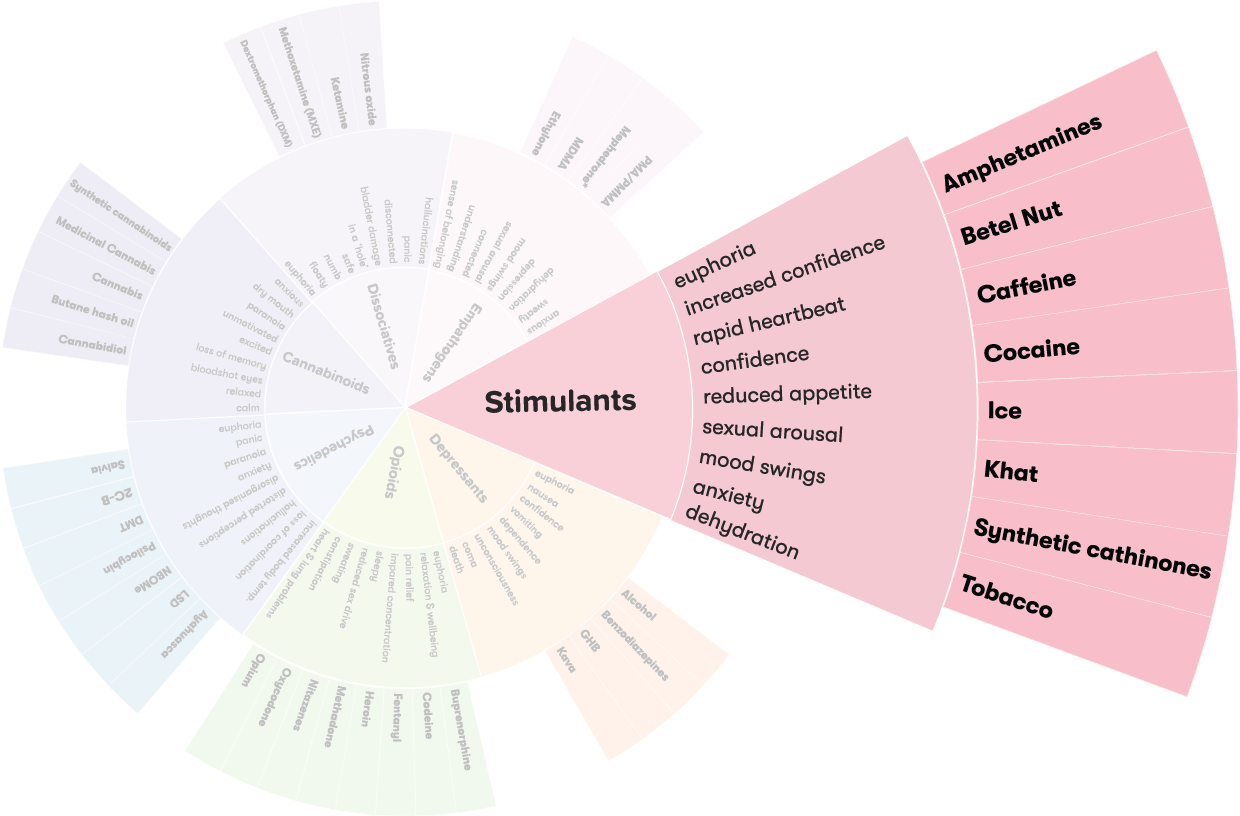
Effects of amphetamines
Use of any drug can have risks. It’s important to be careful when taking any type of drug. .
Amphetamines affect everyone differently, based on:
- size, weight and health
- whether the person is used to taking it
- whether other drugs are taken around the same time
- the amount taken
- the strength of the drug (varies from batch to batch with illegally produced drugs).
You might feel the effects of amphetamines immediately (if injected or smoked) or within 30 minutes (if snorted or swallowed). You might experience:
- feeling happy and confident
- talking more and feeling energetic
- large pupils and dry mouth
- fast heartbeat and breathing
- increased blood pressure
- high body temperature
- dehydration
- teeth grinding
- reduced appetite
- nausea and vomiting
- increased sex drive.2,6,9,10
Snorting amphetamines can damage the nasal passage and cause nose bleeds.
If injecting drugs, there is an increased risk of:
- tetanus
- infection
- vein damage and blood clots.11,12
If sharing needles, there is an increased risk of:
- hepatitis B.
- hepatitis C.
- HIV and AIDS.13
Impact of mood and environment
Drugs that affect a person’s mental state (psychoactive drugs) can also have varied effects depending on a person’s mood (often called the ‘set’) or the environment they are in (the ‘setting’):
- Set: a person’s state of mind, previous encounters with drugs, and expectations of what’s going to happen. For example, feelings of stress or anxiety before using amphetamines may result in an unpleasant experience and make those feelings worse.14
- Setting: the environment in which someone consumes amphetamines – whether it’s known and familiar, who they’re with, if they’re indoors or outdoors, the type of music and light. For example, using amphetamines in a relaxed environment may result in a different experience than being in a noisy, crowded place.14
Overdose
If you take a large amount or have a strong batch, you could overdose.
Call triple zero (000) and request an ambulance if you or someone else has any of the following symptoms (emergency services are there to help and can provide instructions over the phone):
- chest pain
- racing heartbeat
- difficulty breathing
- hot, flushed (red) or sweaty skin
- spasms or seizures
- severe agitation, confusion or panic.15,16
Coming down
In the two to four days after amphetamine use, you may be experience:
- restless sleep and exhaustion
- headaches
- paranoia, hallucinations and confusion
- twitching and muscle aches
- fluctuating temperatures
- irritability, mood swings, anxiety and depression.17,18
Long-term effects
Regular use of amphetamines can cause:
- reduced appetite and weight loss
- restless sleep
- dry mouth
- dental problems
- regular colds and flu
- anxiety and paranoia
- depression
- increased risk of heart attack or other heart problems
- increased risk of stroke
- tolerance and dependence on amphetamines
- financial, work and social problems.1,2,6,19
Amphetamine use and mental health
People who use illegal amphetamines are at increased risk of experiencing mental health issues.20
High doses and frequent heavy use can also create a drug-induced psychosis. This can include experiencing delusions, hallucinations and out of character behaviour.20,21
These symptoms usually go away after the person stops using amphetamines.1,4
Tolerance and dependence
People who regularly use amphetamines can become dependent on the drug. They may feel they need amphetamines to go about their normal activities like working, studying and socialising, or just to get through the day. They may also develop a tolerance to it, which means they need to take larger amounts of the drug to get the same effect.17
Mixing amphetamines with other drugs
Mixing amphetamines with other drugs can have unpredictable effects and increase the risk of harm.
- Amphetamines and alcohol: may feel less intoxicated due to stimulant effects of amphetamine. Increases risk of alcohol poisoning.
- Amphetamines and benzodiazepines: can decrease/mask the effects of both drugs. Risk of overdose if one wears off before the other – depending on amount taken.
- Amphetamines and cocaine: can cause anxiety and heart strain which can lead to stroke.
- Amphetamines and MDMA: can cause anxiety, heart strain, and increase toxic effects on the brain.
- Amphetamines and opioids: can increase the risk of heart strain and respiratory arrest.22,10,23
More on Polydrug use
Polydrug use is a term for the use of more than one drug or type of drug at the same time or one after another. Polydrug use can involve both illicit drugs and legal substances, such as alcohol and medications.
Reducing harm
There are ways in which you can reduce the risks associated with using amphetamines:
- Use around people you trust in a safe environment.
- Eat about 30 minutes before use, then every 2-3 hours after use. Smoothies or sports drinks can help replace electrolytes.
- Prescription amphetamines like Dexamphetamine come with their own dosage instructions which should be followed.
- Take regular breaks from physical activity to cool down.
- Stay hydrated. Drink around 250ml (1 cup) of water per hour when resting, or 500ml per hour when active.
- Try to sleep or rest within a 24-hour period to prevent sleep deprivation.
If snorting
- Use personal straws/spoons, not money, to avoid infections or blood-borne viruses.
- Alternate nostrils and take breaks to minimise nasal damage.23
If injecting
- Always use new, sterile injecting equipment (including sterile water)
- Wash hands thoroughly before and after injecting
- Learn and follow safer injecting practices.
- Safely dispose of used injecting equipment
- Consider using a supervised injecting facility.23
Withdrawal
Giving up amphetamines after a long time is challenging because the body needs to get used to functioning without them.
Withdrawal symptoms should settle down after a week and will mostly disappear after a month. Symptoms can include:
- cravings for amphetamines
- increased appetite
- increased sleep
- vivid dreams and nightmares
- exhaustion
- aches and pains
- depression
- confusion and irritability
- anxiety
- paranoia.4,6,24
Getting help
If your use of amphetamines is affecting your health, family, relationships, work, school, financial or other life situations, or you’re concerned about someone else, you can find help and support.
- Call the National Alcohol and Other Drug Hotline on 1800 250 015 for free and confidential advice, information and counselling about alcohol and other drugs
- Help and support services search
To find a service in your local area from our list. Simply add your location or postcode and filter by service type to quickly discover help near you. - If you’re looking for other information or support options, send us an email at [email protected]
Path2Help
Not sure what you are looking for?
Try our intuitive Path2Help tool and be matched with support information
and services tailored to you.

Use of meth/amphetamines is against the law. Australian Federal and State laws provide penalties for possessing, using, making, selling, importing or exporting, or driving under the influence of meth/amphetamines.
The importation or exportation and the procuring of precursor drugs (such as pseudoephedrine) with the intention of manufacturing a controlled drug, is also against the law. Laws have been introduced that prevent the sale and possession of ice pipes in some states and territories.18
See also, drugs and the law.
- In 2023, 7.5% of Australians had used meth/amphetamines at least once in their lifetime (approximately 1.6 million people).
In 2023, 1.0% of Australians had used meth/amphetamine in the last 12 months. - The average age that Australians first try meth/amphetamine is 22.
- The age group most likely to use meth/amphetamine is 40-49 year olds.
- The main forms used are: crystal/ice - 43%, powder/speed – 31%.
- In 2022, 90% of drug overdose deaths involving amphetamines were unintentional.26, 27
- Darke S, Lappin J, Farrell M. The Clinician's Guide to Illicit Drugs and Health Great Britain: Silverback Publishing; 2019 [cited 26.11.2024].
- Upfal J. Australian drug guide: the plain language guide to drugs and medicines of all kinds. Carlton, Vic, Australia: Black Inc., an imprint of Schwartz Publishing Pty Ltd; 2016 [cited 26.11.2024].
- Castells X, Blanco-Silvente L, Cunill R. Amphetamines for attention deficit hyperactivity disorder (ADHD) in adults. Cochrane Database Syst Rev. 2018; 8:CD007813-CD. [cited 17.10.2024]
- Ruiz P, Strain EC, Langrod JG. The Substance Abuse Handbook. Philadelphia: Wolters Kluwer Health; 2007 [cited 26.11.2024].
- Preedy VR. Neuropathology of drug addictions and substance misuse: Volume 2, Stimulants, club and dissociative drugs, hallucinogens, steroids, inhalants, and international aspects. Amsterdam: Academic Press; 2016 [cited 26.11.2024].
- Campbell A. The Australian illicit drug guide: every person's guide to illicit drugs - their use, effects and history, treatment options and legal penalties. Melbourne: Black Inc; 2001 [cited 26.11.2024].
- Marshman JA, Brands B, Sproule B, Jacobs MR. Drugs & drug abuse: a reference text. Toronto: Addiction Research Foundation; 1998 [cited 26.11.2024].
- Health Direct. Dexamfetamine (Aspen). 2023 [cited 22.10.2024]
- Bapat M. Amphetamine Addiction: Uses, Side Effects, and Treatment. American Addiction Centers; 2024 [cited 22.10.2024]
- Psychonaut Wiki. Amphetamine 2024 [cited 17.10.2024]
- Colledge S, Larney S, Bruno R, Gibbs D, Degenhardt L, Yuen WS, et al. Profile and correlates of injecting-related injuries and diseases among people who inject drugs in Australia. Drug and alcohol dependence. 2020; 216:108267-. [cited 17.10.2024]
- Hahné SJM, White JM, Crowcroft NS, Brett MM, George RC, Beeching NJ, et al. Tetanus in injecting drug users, United Kingdom. Emerg Infect Dis. 2006; 12(4):709-10. [cited 17.10.2024]
- Degenhardt L, Charlson F, Stanaway J, Larney S, Alexander LT, Hickman M, et al. Estimating the burden of disease attributable to injecting drug use as a risk factor for HIV, hepatitis C, and hepatitis B: findings from the Global Burden of Disease Study 2013. Lancet Infect Dis. 2016; 16(12):1385-98. [cited 17.10.2024]
- Nutt D. Drugs without the hot air : making sense of legal and illegal drugs. Cambridge: UIT Cambridge Ltd; 2012 [cited 26.11.2024].
- Schuckit MA. Drug and alcohol abuse : a clinical guide to diagnosis and treatment. New York, NY: Springer; 2006 [cited 22.10.2024].
- Darke S, Lappin, J. & Farrell, M. The Clinician's Guide to Illicit Drugs. United Kingdom: Silverback Publishing 2019 [cited 26.11.2024].
- MedlinePlus USNLoM. Substance use - amphetamines. 2024 [cited 15/10/2024]
- Psychonaut Wiki. Amphetamine. 2024 [cited 16/10/2024]
- Government of Western Australia Mental Health Commission. Harm Reduction Tip Sheet for Workers - Amphetamines. n.d. [cited 17.10.2024]
- McKetin R, Leung J, Stockings E, Huo Y, Foulds J, Lappin JM, et al. Mental health outcomes associated with the use of amphetamines: A systematic review and meta-analysis. EClinicalMedicine. 2019; 16:81-97. [cited 17.10.2024]
- Shoptaw SJ, Kao U, Ling W. Treatment for amphetamine psychosis. Cochrane Database of Systematic Reviews. 2009; (1). [cited 16.10.2024]
- Hi-Ground. Amphetamines n.d. [cited 17.10.2024]
- Harm Reduction Victoria. Speed. [cited 15.10.2024]
- Lintzeris N, Turning Point ADC. Getting through amphetamine withdrawal : a guide for people trying to stop amphetamine use1996. [cited 26.11.2024]
- DRUGS, POISONS AND CONTROLLED SUBSTANCES ACT 1981 - SECT 36B, (n.d.).
- Chrzanowska A, Man N, Sutherland R, Degenhardt L, Peacock A. Trends in overdose and other drug-induced deaths in Australia, 2003-2022. Sydney: National Drug and Alcohol Research Centre,; 2024 [cited 15.10.2024]
- Australian Institute of Health and Welfare. National Drug Strategy Household Survey 2022–2023: Methamphetamine and amphetamine in the NDSHS. 2024 [cited 25.09.2024]