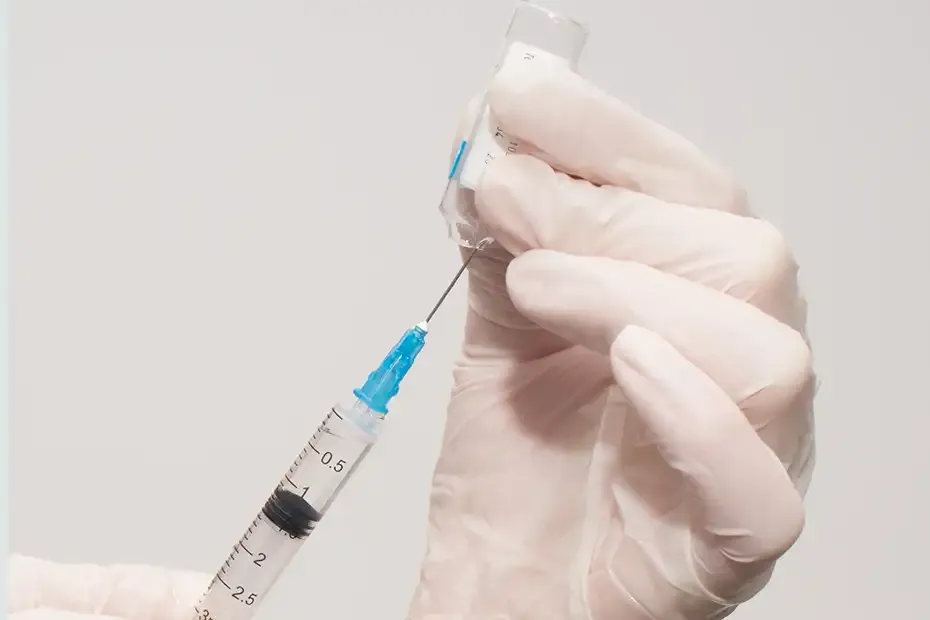
How is it used?
Buvidal® Weekly/Monthly
Buvidal Weekly and Monthly injections are provided in a hospital, clinic or pharmacy by a healthcare professional. This medicine is available only with a doctor's prescription.5
Before beginning Buvidal Weekly or Monthly, you will need to be stabilised on sublingual (placed under the tongue) buprenorphine or buprenorphine/naloxone for at least seven days.5
You can start taking Buvidal Weekly or Monthly the day after your last dose of sublingual treatment.
Your doctor or health care provider will prescribe the correct starting dose of Buvidal Weekly or Monthly for you.5 During treatment , your doctor may decrease or increase the dose according to your needs. If required, you can receive additional doses of Buvidal Weekly during the dosing period.5
How it will be given
Buvidal Weekly or Monthly is injected under the skin (subcutaneously) in the buttock, thigh, abdomen or upper arm.
Sublocade®
Similar to Buvidal Weekly and Monthly, you will need to be stabilised on sublingual (placed under the tongue) buprenorphine or buprenorphine/naloxone for at least seven days before treatment with Sublocade. It comes as a prefilled syringe that is administered by a GP or other health care professional.6
Please be aware
Long-acting buprenorphine formulations are designed to be administered subcutaneously (under the skin). Injecting long-acting buprenorphine formulations like Buvidal® and Sublocade® into a vein can lead to improper release and absorption of the medication, which could result in serious harm or death.
How effective is it?
Treatment with Buvidal or Sublocade is more likely to be successful if it is part of a comprehensive treatment program, which addresses the body, mind and environment in which opioids have been used.
For example, treatment may include a combination of buprenorphine, counselling, alternative therapies and the development of a positive support network of peers, friends and a support group.7
Advantages of buprenorphine maintenance over heroin use
Using buprenorphine on its own is unlikely to result in an overdose. Buprenorphine maintenance keeps the person stable while they make positive changes in their lives. Health problems are reduced or avoided, especially those related to injecting, such as HIV, hepatitis B and hepatitis C viruses, skin infections and vein problems.8
Doses are required only weekly or monthly because the effects are long lasting. Buprenorphine is much cheaper than heroin.8
Effects of buprenorphine
Use of any drug can have risks. It’s important to be careful when taking any type of drug. Even medications can produce unwanted side effects.
Buprenorphine affects everyone differently, based on:
- size, weight and health
- whether the person is used to taking it
- whether other drugs are taken around the same time
- the amount taken.
Side effects
Some of the most common side effects reported with the use of buprenorphine were:
- difficulty sleeping, anxiety
- fatigue, weakness, numbness
- pain in the abdomen, back, arms, legs, joints and muscles, leg cramps, muscle weakness
- flu-like symptoms such as chills, fever, sore throat, coughing, runny nose and sweating
- upset stomach and diarrhoea
- reactions at the injection site (redness, pain, itching, nodule just under the skin)
- abnormal liver function.5, 6
Other less common side effects include:
- dental problems
- headache, migraine
- sleepiness, dizziness, fainting, vertigo
- abnormal vision
- difficulty sleeping
- chest pain
- pain in joints, muscles, back, stomach
- cramps
- flushing, feeling of warmth
- difficulty breathing
- cough, respiratory infection
- nausea, vomiting, constipation
- diarrhoea, poor appetite
- rash and itching
- low sex drive, impotence
- urinary tract infection.5, 6
If you think you are experiencing any of the above side effects, or any other side effects, you should tell your doctor immediately.
Using buprenorphine without a prescription from a doctor, or selling or giving it to someone else, is illegal in Australia. There are also laws against forging or altering a prescription or making false representation to obtain buprenorphine or a prescription for it.7
See also, drugs and the law.
Pharmacotherapy drugs (methadone, buprenorphine and naloxone)
On a snapshot day in mid-2017, nearly 50,000 people in Australia were on a course of pharmacotherapy treatment for their opioid dependence.60% received methadone, 25% received buprenorphine–naloxone and 15% received buprenorphine.8
- NSW Health. Depot buprenorphine 2020 [25.08.2020]. Available from:
- NSW Users and AIDS Association. Depot Buprenorphine: Frequently asked questions n.d. [25.08.2020].
- Victorian State Government. Brief clinical guidelines for use of depot buprenorphine (Buvidal® and Sublocade®) in the treatment of opioid dependence 2020 [25.08.2020].
- Indivior Pty Ltd. Once monthly Sublocade (burprenorphine extended-release) Injection for subcutaneous use 2020 [25.08.2020].
- Camurus Pty Ltd. Buvidal Weekly 2019 [25.08.2020].
- Indivior Pty Ltd. Sublocade® 2020 [25.08.2020].
- Gowing L AR, Dunlop A, Farrell M, Lintzeris N,. National Guidelines for Medication-Assisted Treatment of Opioid Dependence. Department of Health 2014 [25.08.2020].
- A. W. Drug treatment for opioid dependence 2001